The National Health Service (NHS) is investing heavily in diagnostics. Through Getting it Right First Time (GIRFT) and the rollout of Community Diagnostic Centres (CDCs), millions of patients are getting scans more quickly than ever[1]. The NHS 10 Year Plan has now gone further, signalling a major shift in how care will be organised by introducing Neighbourhood Health Centres (NHCs) – local hubs that bring together diagnostics, outpatient clinics, mental health services, and community care under one roof[2].
These initiatives are ambitious, and they are beginning to reshape access to diagnosis. The expansion of imaging capacity has been one of the NHS’s most significant achievements in recent years, shortening waits and enabling earlier detection across a range of conditions. In a service where around 80 percent of patient pathways depend on imaging, continued investment in diagnostics remains essential and deserves recognition – it is the foundation of modern care. To realise its full value, the ability to diagnose more must be matched by the capacity to intervene more. Without equal investment in the systems, teams and spaces that deliver image-guided treatments, the NHS risks creating a new bottleneck: a diagnostic revolution that stalls at the point of intervention.
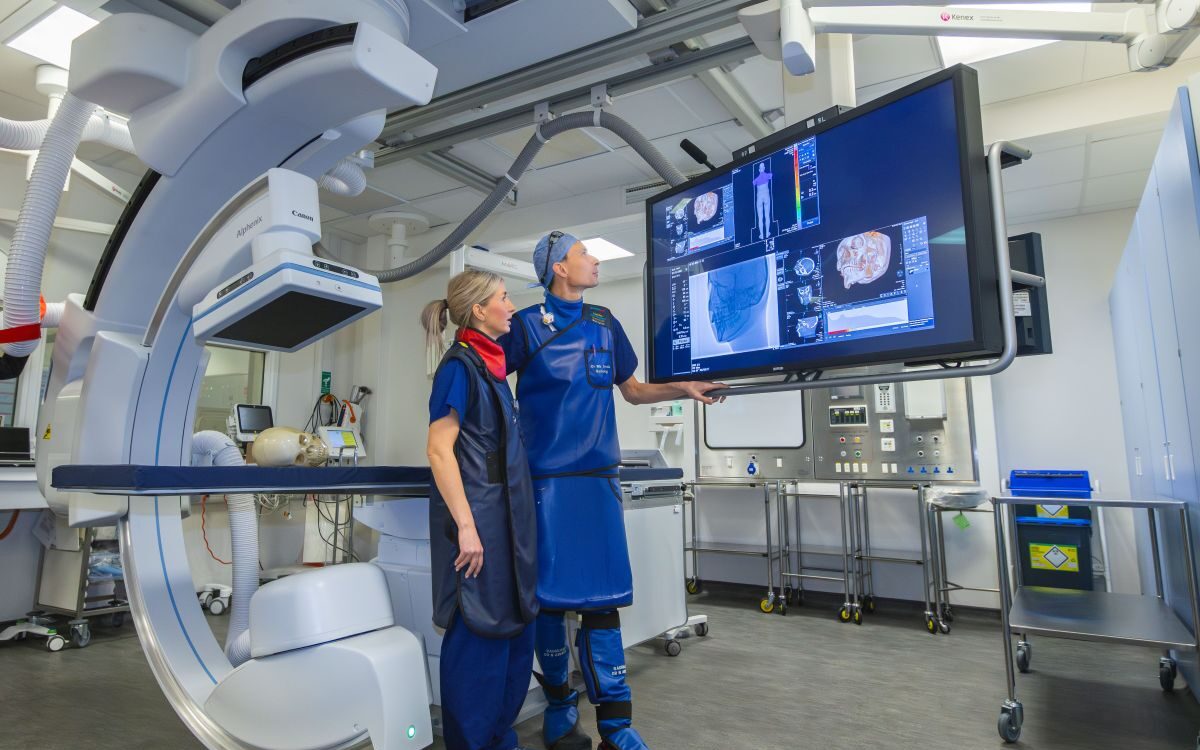
Interventional radiology (IR), the specialty that delivers image-guided, minimally invasive treatments, is the natural partner to the diagnostic surge. Yet the infrastructure, workforce, and commissioning frameworks for IR have not kept pace. The result is an ‘interventional gap’ – a growing disconnect between faster diagnosis and slower access to the procedures that could save lives, salvage limbs, and shorten recovery.
When Scans Outpace Treatment
The Royal College of Radiologists (RCR) census showed a 4.2 percent growth in the radiology consultant workforce in 2024, while CT and MRI demand rose by 8 percent over the same period, underscoring how diagnostic demand continues to outpace workforce capacity[3]. Every interventional case depends on these scans, but also requires anaesthetic support, fluoroscopy rooms, recovery bays, and dedicated staff. The British Society of Interventional Radiology (BSIR) has warned repeatedly that consultant numbers – growing at only around two percent – are far below what is needed to meet the rising complexity of cases and the push for 24/7 healthcare[4].
The patient impact of this gap is stark. In Peripheral Artery Disease (PAD), national registry data still show major amputations at levels that reflect late intervention[5]. Despite National Institute for Health and Care Excellence (NICE) guidance, patients are too often delayed by slow access to duplex ultrasound or computed tomography angiography, or by a lack of available interventional theatre slots. For some, revascularisation arrives too late to save the limb. In stroke, mechanical thrombectomy can prevent severe disability if delivered quickly, yet services remain patchy, and round-the-clock cover is not universal[6]. In oncology, minimally invasive ablation and embolisation offer alternatives to surgery; however, limited day-case capacity means patients wait longer than necessary, sometimes ending up in hospital through emergency routes rather than planned care.
Neighbourhood Health Centres as a Missed or Seized Opportunity
The rapid build-out of CDCs was designed around diagnostics, not treatment. These centres are already delivering millions of scans, but most lack the fluoroscopy suites, recovery bays, and procedure capacity required for IR[7]. The 10 Year Plan’s Neighbourhood Health Centres are set to go further by integrating diagnostics with outpatient clinics, physiotherapy, mental health support, and social care[8]. The promise to make healthcare more local and more joined-up is good. However, unless IR is considered from the outset, ensuring that diagnostic pathways flow directly into interventional capacity, the same pattern may repeat itself: faster scanning, but an unchanged treatment queue.
Workforce is another constraint. Consultant numbers in interventional radiology are not expanding fast enough, and uneven rotas for out-of-hours cover place pressure on a small pool of specialists. The Royal College of Radiologists (RCR) shows that while consultant numbers rose by 6.3 percent in 2023, demand for imaging grew nearly twice as fast, forcing the NHS to rely heavily on locums and outsourcing to private providers and insourcing agencies[9]. This offers short-term relief but undermines continuity and training, a concern also raised in the British Society of Interventional Radiology’s (BSIR) service provision strategy[10].
To counter these gaps, the NHS is beginning to embrace new workforce models. Advanced Practice Radiographers can take on key tasks such as pre-assessment, vascular access, and post-procedure review, which frees consultants to focus on delivering more interventions[11]. Nurse-led triage and pre-operative optimisation clinics have also been shown to reduce same-day cancellations and improve patient flow, helping Trusts make full use of existing day-case slots. These innovations are encouraging, but adoption remains inconsistent, and they need proper governance and investment if they are to become a genuine part of the solution.
Commissioning and policy are the third factor. Diagnostics have benefitted from clear national frameworks, funding streams, and measurable targets. Intervention has not. There is still no comprehensive national registry capturing the breadth of IR procedures, from uterine fibroid embolisation (UFE) to prostate artery embolisation (PAE), from oncology ablation to limb salvage. Without robust data, IR remains less visible in policy conversations. Tariffs often fail to reward minimally invasive, day-case procedures, leaving Trusts with little incentive to prioritise them over more resource-intensive surgery. While the 10-Year Plan sets ambitious goals for community-based care, it may not achieve them unless interventional services are commissioned as an integral part of the neighbourhood delivery.
What Closing the Gap Could Deliver
The benefits of closing the interventional gap are profound. Elective recovery would accelerate if day-case IR procedures could be scaled up across the country, reducing reliance on general theatres and cutting waiting times. Inequalities could be reduced by embedding chronic limb-threatening ischaemia and high-risk foot pathways into every Integrated care system, ensuring patients in deprived communities get timely access to revascularisation rather than late amputations[12]. The NHS’s commitment to value-based care would be advanced because IR procedures often result in shorter hospital stays, fewer complications, and faster return to independence.
So, how can the NHS move from diagnostics to a complete pipeline of diagnosis and intervention? It must embed IR into the design of CDCs or Neighbourhood Health Centres from the outset, ensuring they offer not only scans and outpatient appointments but also day-case suites with the recovery capacity to deliver common procedures locally. It must redesign the workforce model to expand the role of advanced practitioners and increase training posts to incentivise consultants to work across regions, particularly those underserved by specialist care. It must align commissioning with outcomes through tariffs that reward minimally invasive procedures, mandatory metrics on time-to-revascularisation and day-case conversion rates, as well as funded registries to track quality and equity. It must treat IR as a strategic priority in the same way diagnostics have been treated – with clear targets, sustained investment, and national leadership.
From Diagnosis to Cure
The NHS is right to celebrate its diagnostic advances, but diagnosis is only the beginning. A patient who can access a scan within days but must wait months for treatment is not receiving the full benefit of modern healthcare. The promise of the NHS 10-Year Plan and the Neighbourhood Health Centres lies in care that is joined-up, local, and efficient. That promise will only be realised if intervention keeps pace with diagnostics.
Closing the interventional gap is not just about protecting a specialty; it is about ensuring that the NHS’s new diagnostic and community models deliver on their ultimate purpose: better outcomes for patients. Diagnosis without timely treatment is a half-finished story. The NHS has shown it can scale diagnostics with urgency and ambition. Now it must do the same for intervention, so that every scan is not just an image of disease, but the first step on a clear path to cure.
Author Bio

Dan Parr, Imaging Systems Business Manager, Canon Medical Systems UK
- Author name – Dan Parr
- Professional background – Medical imaging professional with over fifteen years of clinical and industry experience.
- Role at Canon Medical Systems UK – Imaging Systems Business Manager
- LinkedIn profile link – Daniel Parr | LinkedIn
Disclaimer: Dan Parr is Imaging Systems Business Manager at Canon Medical Systems UK, a company that manufactures and supplies interventional radiology and diagnostic imaging equipment to NHS and private healthcare providers. While this article contains no reference to Canon Medical products or services, readers should be aware that the author has a professional and commercial interest in the expansion of interventional radiology services within the NHS.