Are we mistaking associations for true biological origins?
Despite significant advances in modern medicine, lifestyle diseases such as cardiovascular disease and diabetes continue to rise globally. These conditions are commonly described as “multifactorial,” attributed to a combination of diet, genetics, stress, sleep, and other variables. While this framework has been useful in identifying risk patterns, it may represent an incomplete understanding of disease causation.
A critical distinction that often goes unexamined is the difference between statistical association and biological causation.
In current medical thinking, risk factors are frequently treated as primary drivers of disease. However, an associated factor may not necessarily represent the initiating cause. As I often describe it, an associated factor is like a witness to an event—not the origin of it.
For instance, elevated LDL cholesterol is strongly associated with cardiovascular disease. Clinically, managing such markers plays an important role in reducing immediate risk and guiding treatment decisions. However, the presence of an association does not, by itself, explain the underlying biological processes that give rise to the condition.
This distinction has been recognized within the scientific community. Glass and McAtee have described the growing limitations of traditional risk factor epidemiology, pointing to what they term “causal ambiguity,” where associations are identified, but deeper mechanistic understanding remains unclear. Similarly, Vandenbroucke and colleagues have cautioned against conflating statistical correlations with true causation.
This brings us to what can be described as the “Firefighter Fallacy.” Observing firefighters at the scene of a fire does not imply they caused it. In the same way, identifying biomarkers associated with disease does not necessarily reveal the origin of the pathology. If interventions focus solely on modifying these markers without addressing underlying processes, we may be managing outcomes rather than resolving causes.
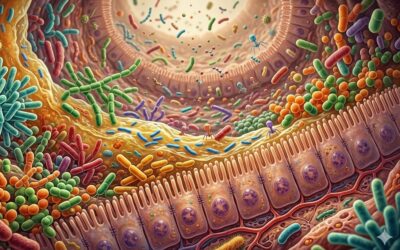
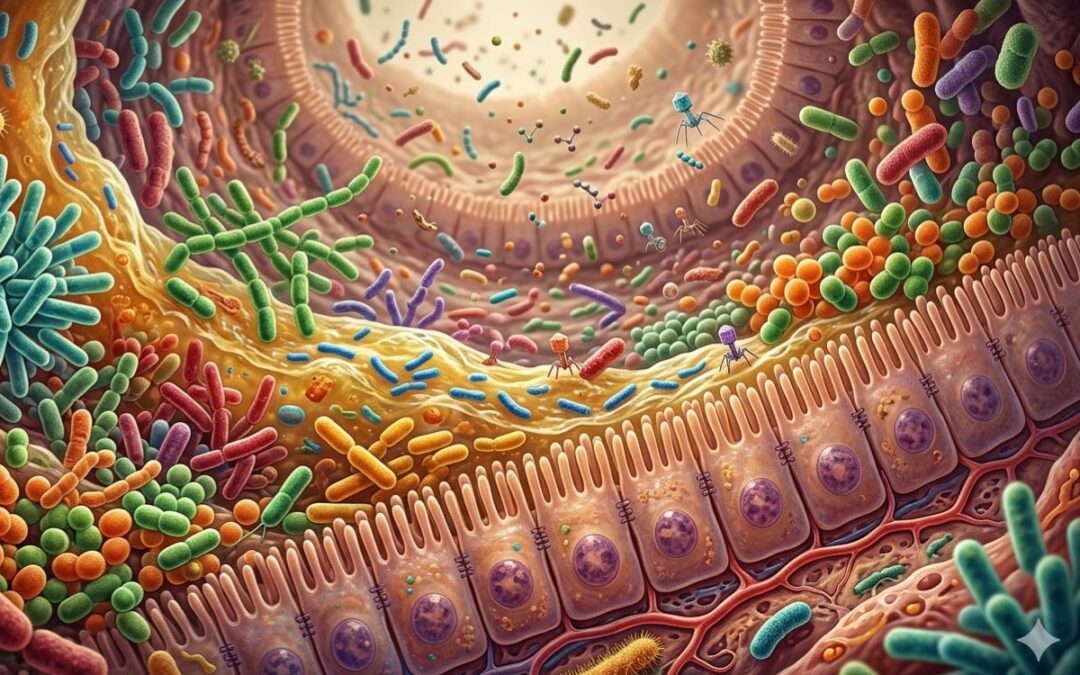
A more comprehensive approach may lie in shifting attention toward cellular-level processes and systems biology. Disease does not originate at the level of population statistics; it begins with changes in cellular function, tissue integrity, and biochemical balance. Understanding these foundational processes—what might be termed cellular pathogenesis—could provide deeper insight into why certain patterns, such as altered lipid profiles or impaired glucose metabolism, emerge.
This perspective does not dismiss the importance of lifestyle factors such as diet, physical activity, and sleep. On the contrary, these remain essential components of health. However, their role may be better understood not just as isolated risk modifiers, but as influences on underlying biological systems.
The key shift, therefore, is conceptual. It is a move from managing measurable indicators to exploring the origins of dysfunction. When causation is understood at a fundamental level, interventions can become more targeted, coherent, and potentially transformative.
In an era of increasing chronic disease burden, refining our understanding of causation may be just as important as advancing treatment. The challenge is not only to identify what is associated with disease, but to ask a deeper question:
Are we addressing the true origin of the problem—or its visible signals?
Author Bio

Dr. Balaram Dhotre
Dr. Balaram Dhotre is an author and disease reversal nutritionist focused on understanding the root causes of lifestyle diseases through nutrition and cellular health perspectives. His work explores the distinction between statistical associations and biological causation in chronic disease.