In cardiology and diabetes, we no longer rely on single, in-clinic readings to diagnose complex conditions; instead, remote monitors are used to capture data over a period of time. We’ve seen that the standard of care across medicine is shifting from episodic “snapshots” to continuous Remote Patient Monitoring (RPM). However, in reproductive health, we are still largely operating in the analog era.
Current fertility diagnostics rely heavily on binary, isolated data points:
- a urinary LH test to predict ovulation (Yes/No),
- or a single serum progesterone draw—often scheduled on “Day 21″—to confirm it.
While standard, these tools are fundamentally limited. They capture a moment in time, but they miss the movie.
The future of fertility care lies in continuous, passive, and clinically validated remote monitoring. This shift is not just about convenience; it is about closing a massive diagnostic gap that “snapshot” medicine has left open.
The Clinical Consequence: Missing the “Silent” Pathology
The menstrual cycle is a dynamic hormonal event. The standard practice of testing progesterone seven days post-ovulation assumes a “textbook” 28-day cycle that few women (less than 15%) actually have.
If a patient ovulates on Day 18, a Day 21 blood test is premature, which could potentially lead to a false diagnosis of anovulation. More critically, a single blood draw provides only a snapshot of the quality of the luteal phase, if timed correctly, but cannot show the duration of the luteal phase, which can be reflective of the hormone quality too. It cannot detect a “slow rise” in progesterone or a premature drop—subtle patterns that characterize Luteal Phase Deficiency (LPD), a leading cause of unexplained infertility and recurrent miscarriage.
To catch these nuances, we don’t need a sharper snapshot; we need continuous footage.
Validating the “Lab at Home.”
The barrier to adopting RPM in fertility has historically been data quality. Clinicians have been right to be skeptical of consumer wearables that measure peripheral temperature (wrist or finger), which is susceptible to environmental noise and vasoconstriction.
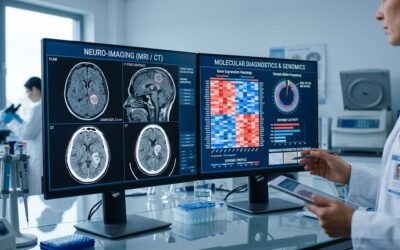
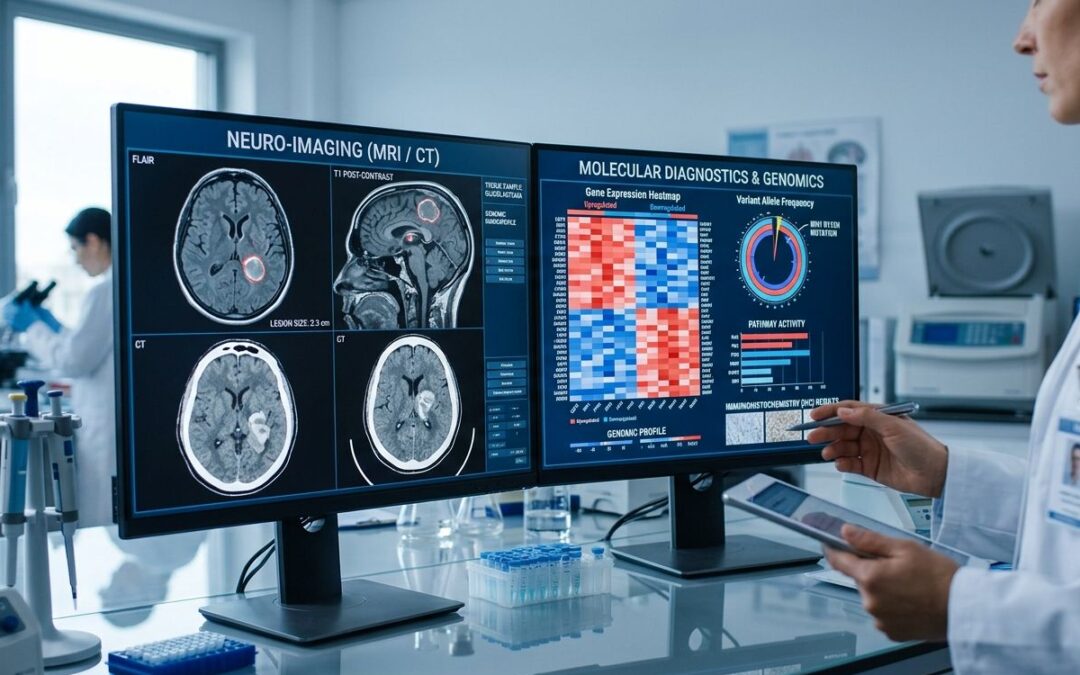
However, the landscape has changed. A 2025 validation study published in the peer-reviewed journal Sensors analyzed 194 cycles across 125 women using a continuous axillary temperature sensor. The study compared the wearable’s data against the gold-standard urinary LH surge.
The results were pivotal for the RPM model:
- The sensor identified ovulation with comparable accuracy to urinary LH tests.
- It successfully identified the retrospective biphasic pattern necessary to confirm not just that ovulation occurred, but that the corpus luteum was functioning.
- Critically, algorithmic filtering of environmental noise and sleep disturbances proved successful in making the data viable for postpartum patients and shift workers—populations previously excluded from accurate tracking.
The Economic and Clinical Upside
Moving fertility diagnostics out of the clinic and into the home offers a dual benefit.
- For the Clinician: It provides a longitudinal “digital biomarker.” Instead of relying on a patient’s memory or a paper chart with potentially missing data, the physician logs in to a portal and sees months of clean, overlaid cycle data. They can visually verify if a progesterone prescription is lengthening the luteal phase, or if lifestyle interventions are regulating ovulation.
- For the Patient: It reduces the burden of care. Continuous monitoring removes the need for timed intercourse based on stressful urine strips or invasive clinic visits for blood monitoring.
The era of the “Day 21” snapshot is closing. Just as cardiology and endocrinology have embraced continuous data, reproductive medicine is now poised to follow. With validated clinical data, continuous remote monitoring now offers the potential to treat the menstrual cycle with the precision of a true vital sign, providing clinicians with better data and subsequently patients with better care.
Author Bio
Michael Vardi is the Founder and CEO of Tempdrop. Holding an M.Sc. in Biomedical Engineering from Tel-Aviv University, Michael has a deep background in medical device development and digital health. His work focuses on the application of continuous basal body temperature data and algorithmic analysis for remote cycle monitoring.