Alzheimer’s disease (AD) represents a significant medical concern for all of us as we grow older, as the NIH has published that the average risk of dementia over 55 years old is now 42%. AD is presently affecting 6.9 million Americans aged 65 or older and is expected to grow to 13.8 million Americans by 2060, affecting an estimated 55 million people worldwide. AD is a major public health concern.
On top of a growing problem with AD, we have an overlapping Lyme disease epidemic, where Lyme disease (LD), due to an infection with Borrelia burgdorferi (Bb) is spreading worldwide with global Bb seroprevalence estimated at 14.5%. Roughly 33% of those infected with Bb may go onto develop chronic persistent symptomatology despite treatment with antibiotics, known as ‘Chronic Lyme disease (CLD)/Post Treatment Lyme Disease Syndrome (PTLDs). Symptoms of CLD/PTLDs oftentimes overlap those of other chronic fatiguing, musculoskeletal, cardio-pulmonary, neuropsychiatric illnesses including Chronic Fatigue Syndrome (CFS)/Myalgic Encephalomyelitis (ME), Fibromyalgia (FM), Long Covid (LC), mold toxicity and Alzheimer’s dementia. Lyme disease is known to cause significant cognitive difficulties and problems with executive functioning, impairing memory and concentration. We have two overlapping epidemics and one of them involves a spirochetal infection known to cause AD-like changes in the brain and memory problems. I believe that one epidemic is likely significantly affecting the other. My hypothesis is based on the following:
The scientific literature has shown a strong association between an infection with Lyme disease, Borrelia burgdorferi (Bb) and Alzheimer’s like changes in the brain. This has been published multiple times in the peer-reviewed literature, including in the Journal of Alzheimer’s Disease (JAD). In a meta-analysis of case controlled studies, there was greater than a ten-fold increased occurrence of AD when there was detectable evidence of a spirochetal infection. Lyme is a spirochete like syphilis, a known cause of dementia. This connection is also consistent with prior research showing that amyloid-β has anti-microbial properties. Researchers have found production of biofilm, amyloid plaques and phosphorylated tau tangles around spirochetal infections on brain biopsies of autopsied patients with chronic Lyme disease who died from either Parkinson’s or AD. The association of an infection driving amyloid-beta and p-tau, i.e., the infection/amyloid/p-tau hypothesis, has remained a hypothesis up until now primarily because the association was based on numerous autopsy studies. Association does not equal causation, especially when no one had ever reported reversing Alzheimer’s biomarkers with an antibiotic protocol in a live patient, proving that it was in fact an infection increasing amyloid-beta and phosphorylated tau. Until now.
I just published a case report in the Journal of Alzheimer’s Disease Reports where I completely reversed p-tau and improved amyloid-beta ratios by addressing multiple sources of inflammation, and in this case, I did it by treating a Lyme infection present in my patient for the past 15 years. One of the holy grails in medicine has been to find a potential solution for Alzheimer’s disease and this study gives us at least a glimmer of hope. Why?
A Cochrane review published several weeks ago on the efficacy and safety of anti-amyloid monoclonal antibodies used to treat AD determined that they were helpful in slowing down the disease process, although they were insufficient to significantly change the clinical course of AD with potential side effects. The Cochrane review suggested the need for further research in other areas. One week later, I published a scientific study in the Journal of Alzheimer’s Disease Reports reporting for the first time the reversal of P tau 217, the most sensitive and specific biomarker for AD in a patient with chronic Lyme disease (CLD)/Post Treatment Lyme Disease Syndrome (PTLDS) with a short-term antibiotic protocol while improving beta-amyloid ratios. You can read the study here:
Improving biomarkers of inflammation including phosphorylated tau in a patient with chronic Lyme disease/post-treatment Lyme disease syndrome using dapsone combination therapy: A case study and literature review. Richard Horowitz. Review article. Journal of Alzheimer’s Disease Reports. First published online April 27, 2026 https://journals.sagepub.com/doi/10.1177/25424823261445434
While anti-amyloid monoclonal antibodies have been shown to have the ability to lower p-tau 217 by an average of 23% over 6 or more years, an 8-9 week oral, generic, biofilm/persister antibiotic protocol, i.e., dapsone combination therapy (DCT) was able to lower p-tau 217 by 63% in 8-9 weeks and completely reverse it back into normal range. This had never been accomplished and DCT did this while lowering down a marker of peripheral inflammation, rheumatoid factors (RF). Rheumatoid factors are not specific for Rheumatoid Arthritis (RA) as several infections and diseases may elicit RFs. Prevalence studies of RF positivity in infections have highlighted that chronic, constant exposure to microbial antigens are needed for the development of RFs.
The reason some of our anti-amyloid monoclonal antibodies are having limited success may therefore be due to some individuals having a chronic, persistent biofilm infection, like Bb increasing amyloid-beta and p-tau. Or they have other infections. In my case study, I addressed other infections (Coxiella burnetii, Babesia microti, Bartonella species), environmental toxins (heavy metals), vitamin deficiencies, intestinal hyperpermeability and metabolic syndrome. I addressed overlapping sources of inflammation to ensure the best clinical outcome.
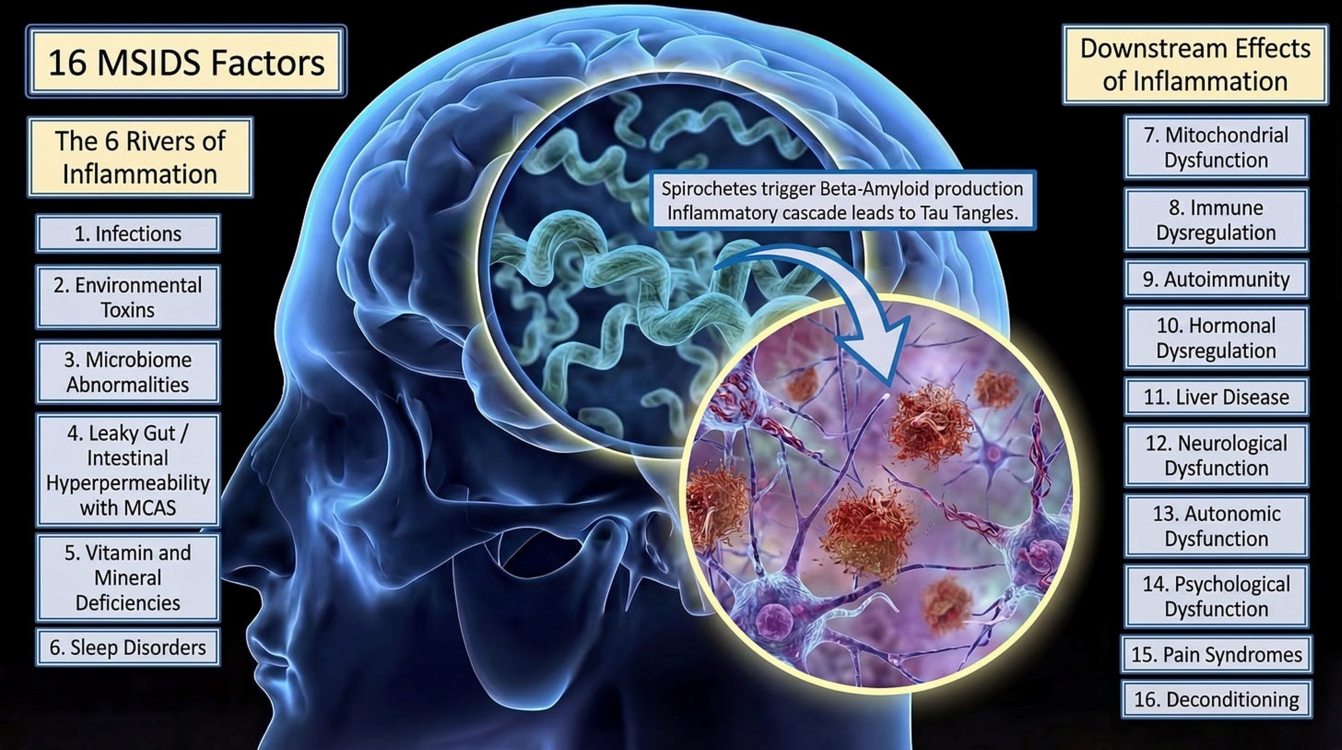
This case study highlights a new avenue for AD research. Not only should we do research on the efficacy and safety of DCT for the treatment of AD patients who have been exposed to Bb, but the framework in this article outlines that multifactorial causation may underlie the dementia process. I found that all 16 of the inflammatory factors that I have published to potentially underlie cases of CLD/PTLDS and Long Covid, now also applies to AD. It brings together the different hypotheses that have been proposed to account for the AD epidemic including the “amyloid cascade hypothesis, tau hypothesis, neuroinflammation hypothesis, cholinergic hypothesis, mitochondrial dysfunction hypothesis, vascular hypothesis, along with emerging theories involving infectious agents, neurotoxicity (Al, Hg, pesticides), cholesterol dis-metabolism, brain insulin resistance, white matter injury and dysbiosis in the gut microbiome affecting the gut/brain axis”.
Discovering that 16 potential underlying inflammatory factors may underlie AD pathology, especially in some cases, spirochetal infections like Borrelia burgdorferi…provides clues to the next steps in the scientific communities quest to find a solution. We must conduct scientific research with placebo-controlled, multicenter, randomized controlled trials of dapsone combination therapy and the 16 MSIDS factors in both CLD/PTLDs and Alzheimer’s patients. One arm of the study could include Alzheimer’s patients with elevated AD biomarkers who have been screened for these 16 MSIDS factors and found to have prior exposure to Lyme disease; the other arm could be chronic Lyme patients with elevated AD biomarkers who are screened for all 16 MSIDS factors and found to have an elevated risk of dementia as they age. We would give these patients DCT (or a placebo) and address MSIDS factors and follow the patients and their AD biomarkers long-term. Based on this being the 11th published article in the peer-reviewed journals on the efficacy of DCT to treat CLD/PTLDS and improve 8 major Lyme symptoms among more than 350 retrospective patients, I am hopeful.
This case study is the first to definitively link an infection with Borrelia burgdorferi, the agent of Lyme disease, with Alzheimer’s disease, indicating that in some cases effectively treating the infection with a biofilm/persister antibiotic regimen and addressing overlapping inflammatory factors may help to decrease both amyloid and phosphorylated tau in the brain. Dapsone also blocks the NLRP3 inflammasome, a key driver of chronic neuroinflammation. Repurposing of dapsone in AD may be warranted with so few solutions.
Although we cannot generalize from one case study, this study provides a direction for further research which is desperately needed.
Author Bio

Dr. Richard Horowitz, MD
Dr. Richard Horowitz is a board-certified internist and medical director of the Hudson Valley Healing Arts Center, an integrative medical center specializing in the treatment of Lyme and other tick-borne diseases. He has treated over 13,000 Lyme and TBD patients in the last 40 years and is one of the founding members and past president elect of ILADS. Dr Horowitz has published multiple peer-reviewed articles on effective diagnostic and treatment options for Lyme and co-infections and served as a member of the HHS Tick-borne Disease Working Group in 2017-2018. He was also co-chair of the HHS Tick-borne Co-infection subcommittee which gave recommendations to Congress on the prevention, diagnosis, and treatment of tick-borne illness, and he was recently elected to the NYS Department of Health Tick-borne Disease Working Group. For dedicating his life to helping those stricken with this devastating illness, he has been awarded the Humanitarian of the Year award by the Turn the Corner Foundation and awards from Project Lyme. He is the author of multiple books on Lyme disease and chronic illness, including his forthcoming title Ending Chronic Illness, to be published by Simon and Schuster in October 2026.