What Are GLP-1 Receptor Agonists?
GLP-1 receptor agonists have become one of the most talked-about drug classes in modern medicine. Originally developed to treat type 2 diabetes, these medicines now carry approved indications spanning obesity, cardiovascular disease, chronic kidney disease, liver disease, and obstructive sleep apnoea. Understanding what GLP-1 receptor agonists are, how they work at a biological level, and who stands to benefit from them is increasingly relevant not just for clinicians and researchers, but for patients and the wider public navigating a rapidly evolving treatment landscape.
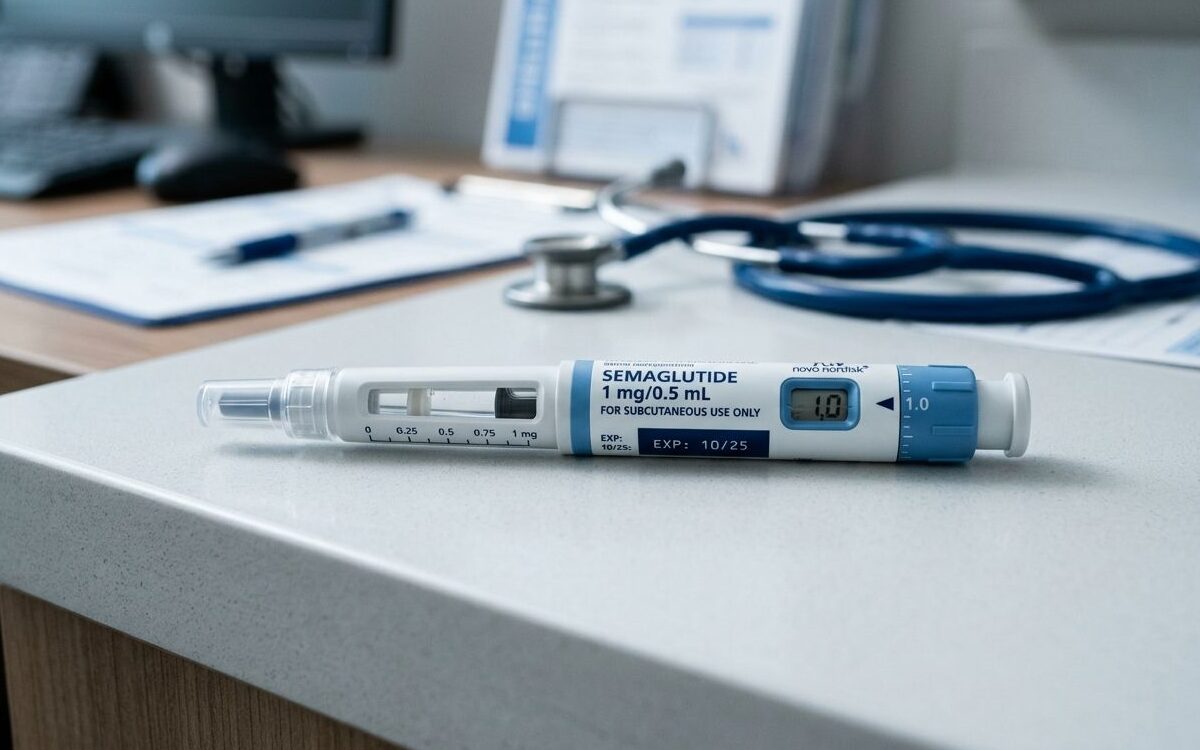
GLP-1 stands for glucagon-like peptide-1, a hormone produced naturally in the L-cells of the distal small intestine in response to eating. It plays a central role in regulating blood glucose by stimulating insulin secretion from the pancreas, suppressing glucagon release, and slowing gastric emptying. GLP-1 receptor agonists are synthetic compounds designed to mimic and prolong these effects, binding to the same receptors as the natural hormone but remaining active in the body for far longer than GLP-1 itself, which is broken down within minutes.
The Biology Behind the Benefits
The GLP-1 receptor is a class B G protein-coupled receptor found across multiple organ systems, including the pancreatic islets, brain, cardiovascular tissues, kidneys, lungs, and gastrointestinal tract. This widespread distribution helps explain why GLP-1 receptor agonists produce effects that extend well beyond blood sugar control.
In the pancreas, these drugs stimulate insulin secretion in a glucose-dependent manner, meaning insulin is only released when blood glucose levels are elevated. This feature significantly reduces the risk of hypoglycaemia compared with older diabetes medicines such as sulphonylureas. At the same time, GLP-1 receptor agonists suppress glucagon, the hormone that signals the liver to release stored glucose into the bloodstream.
In the brain, GLP-1 receptor agonists act on regions that govern appetite and energy balance. By modulating neurotransmitter and peptide release in areas such as the hypothalamus, they reduce hunger signals and enhance the feeling of satiety. This central action, combined with the slowing of gastric emptying that delays the passage of food from the stomach, is central to the weight loss these drugs produce.
Beyond metabolism, GLP-1 receptor agonists exert anti-inflammatory and cardioprotective effects. In the liver, they reduce hepatic fat accumulation and oxidative stress. In the kidneys, they mitigate glomerular hypertension and promote natriuresis. In cardiovascular tissue, clinical evidence demonstrates improved myocardial function and a meaningful reduction in the risk of major adverse cardiovascular events, including heart attack and stroke.
From Diabetes Drug to Multi-System Therapy
The first GLP-1 receptor agonist approved for clinical use was exenatide, derived from a protein found in the saliva of the Gila monster lizard and approved by the US Food and Drug Administration in 2005 for the management of type 2 diabetes. Liraglutide followed in 2010, with dulaglutide approved in 2014, and semaglutide in 2017. Tirzepatide, a dual agonist targeting both the GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) receptors, received FDA approval in 2022 and represented a new generation of incretin-based therapy.
Today, the approved indications for drugs in this class have expanded considerably. Semaglutide, marketed as Wegovy by Novo Nordisk, was approved for chronic weight management in adults with obesity in 2021. The landmark SELECT trial subsequently demonstrated that semaglutide significantly reduced the risk of major adverse cardiovascular events in overweight or obese adults with established cardiovascular disease, leading to a further FDA approval for that indication.
In January 2025, semaglutide (Ozempic) received FDA approval to reduce the risk of kidney failure and disease progression in adults with type 2 diabetes and chronic kidney disease, supported by data from the FLOW trial, which showed a 24% reduction in kidney-related complications compared with placebo. In August 2025, Wegovy became the first GLP-1 receptor agonist to gain FDA approval for metabolic dysfunction-associated steatohepatitis (MASH) with moderate-to-advanced liver fibrosis. Tirzepatide, meanwhile, became the first medication approved for moderate-to-severe obstructive sleep apnoea in adults with obesity in late 2024.
These successive approvals reflect a broader recognition of GLP-1 receptor agonists as multi-system therapeutic agents rather than glucose-lowering drugs alone.
Who Are These Medicines For?
The eligible patient population for GLP-1 receptor agonists has grown substantially, and in the UK, recent regulatory guidance has accelerated that expansion.
For type 2 diabetes, GLP-1 receptor agonists are established treatments when blood glucose remains inadequately controlled despite first-line therapy, or when a patient presents with additional cardiovascular, renal, or weight-related risk factors. The 2025 American Diabetes Association standards of care recommended GLP-1 receptor agonists as first-line pharmacological therapy alongside SGLT2 inhibitors for patients with type 2 diabetes who have or are at high risk of atherosclerotic cardiovascular disease or heart failure.
In the UK, NICE updated its type 2 diabetes management guidelines in early 2026, significantly widening the eligibility criteria. Under the new guidance, GLP-1 receptor agonists are now recommended for people with type 2 diabetes who have cardiovascular disease caused by blocked arteries, those diagnosed with the condition before the age of 40, or those living with obesity. NICE estimated that around 810,000 additional people could become eligible as a result.
For obesity, eligibility in the UK typically follows NICE criteria requiring a BMI of 35 kg/m² or above alongside weight-related comorbidities, though lower thresholds apply for some ethnic groups where obesity-related risk presents at lower BMI levels. NHS access to GLP-1 receptor agonists for weight management has historically been restricted to specialist tier 3 services, reflecting both cost pressures and limited capacity, though this landscape continues to evolve.
Clinical trial data have consistently demonstrated meaningful weight loss across the drug class. Studies have recorded weight reductions of between 7% and 24% of body weight depending on the agent and dose, with tirzepatide producing the highest weight loss figures seen to date among approved medicines. A May 2025 study from FAIR Health reported that more than 2% of US adults were taking a GLP-1 receptor agonist for weight loss in 2024, with awareness among the general public continuing to rise.
Beyond diabetes and obesity, patients with established cardiovascular disease and those with chronic kidney disease co-occurring with type 2 diabetes now represent a defined population for whom GLP-1 receptor agonists carry approved indications. The emerging evidence base in non-alcoholic liver disease, obstructive sleep apnoea, and potentially in neurodegenerative conditions continues to broaden the therapeutic horizon.
Who Should Not Take Them
Not all patients are suitable candidates. GLP-1 receptor agonists are contraindicated in individuals with a personal or family history of medullary thyroid carcinoma or multiple endocrine neoplasia type 2, based on animal study data, although a direct causal link in humans has not been confirmed. They are also contraindicated during pregnancy, and women of reproductive potential should discuss effective contraception with their prescriber before starting treatment.
Patients with a history of pancreatitis require heightened caution, as GLP-1 receptor agonists have been associated with reports of acute pancreatitis, though a definitive causal relationship remains unestablished. The most commonly reported side effects across the class are gastrointestinal, particularly nausea, vomiting, and diarrhoea, which tend to be most pronounced during the dose titration phase. These effects lead to discontinuation in a proportion of patients, though gradual titration schedules are widely used to improve tolerability.
A 2025 study also identified associations between GLP-1 receptor agonist use and increased risks of hypotension, syncope, joint diseases, kidney stones, and interstitial nephritis, underscoring the importance of individual clinical assessment before prescribing. Prescribers should evaluate each patient’s full medical history, concurrent medications, and treatment goals before initiating therapy.
What Comes Next
The pipeline of next-generation agents continues to advance. Orforglipron, the first non-peptide oral GLP-1 receptor agonist, completed Phase III trials in 2025 and, if approved, could remove the injection-related barrier that currently limits access for some patients. Retatrutide, a triple agonist targeting GLP-1, GIP, and glucagon receptors simultaneously, has demonstrated significant weight loss in Phase II trials and is advancing through development. Combination approaches and longer-acting formulations are also under investigation.
The clinical evidence base for GLP-1 receptor agonists has shifted significantly in a short period of time. What began as a single-indication diabetes drug class has expanded into one of the broadest therapeutic platforms in contemporary medicine. As new approvals accumulate, access policies evolve, and next-generation molecules approach the market, GLP-1 receptor agonists are likely to remain central to the treatment of metabolic disease for years to come.